Dry skin is a widespread skin concern. When accompanied by periodic, uncomfortable symptoms like itching, redness, cracked skin, and blisters, it may be a sign of a chronic condition called eczema.
This article explains what eczema is, what triggers symptoms, and how to manage them.

What Is Eczema?
Eczema is a non-contagious, inflammatory skin condition. It is sometimes referred to as atopic dermatitis, the most common type of eczema.
Millions of people worldwide suffer from this condition. It manifests as very dry and sensitive skin that is unable to maintain moisture. Due to compromised barrier function, the skin with eczema typically flares up in response to a host of factors, from environmental pollutants to emotional stress. Thankfully, various treatments can manage symptoms.
Note: Discover how are stress and skin related and what can you do about it.
Types of Eczema
There are seven types of eczema depending on the symptoms, what triggers them, and the age group they typically affect. One symptom they all have in common is – itching.
- Atopic dermatitis – It is the most common eczema type, appearing at an early age but affecting all age groups – especially people who also have asthma, hay fever, or food allergies. Common symptoms include dryness, inflammation, and itching anywhere on the body.
- Seborrheic dermatitis – Also known as dandruff, it usually causes redness and greasy, flaky skin on the scalp, sides of the nose, behind the ears, eyebrows, and upper back. A yeast that lives on the skin’s surface commonly triggers seborrheic eczema.
- Contact dermatitis – The symptoms usually appear after contact with chemical irritants and environmental allergens. Patients experience a burning sensation and discomfort on the spot that touches the irritant – usually the hands.
- Dyshidrotic dermatitis – Intense itching, scaly skin, rashes, blisters, and cracks on the hands and feet commonly occur in patients with this type of eczema. It usually runs in families.
- Nummular dermatitis – Exposure to cold, dry air and chemical irritants brings about red, itchy, round, and sometimes oozing patches of skin on the legs, arms, and torso. Adults are more prone to this type of eczema than children.
- Neurodermatitis – It starts with small, itchy patches on the scalp, behind the ears, on the neck, wrists, ankles, and genitals. They cause patients to scratch, leading to more intense itching and eventually thick, dry, leathery skin. Common triggers include stress, tight clothing, and nerve injury. It mainly affects women between 30 and 50 years of age and people with contact or atopic dermatitis.
- Stasis dermatitis – It causes dry, itchy, scaly skin, discoloration, and swelling on the legs due to poor circulation. It typically affects people over 50.
What Causes Eczema?
The medical community recognizes a complex, interlinked variety of causes. Different eczema types have different causes, but they usually stem from a genetic predisposition combined with external triggers.
Causes of eczema include:
- Family history of atopic dermatitis, hay fever, and asthma.
- Inheriting genes that increase the likelihood of developing dermatitis.
- Deficiency of filaggrin, the protein responsible for retaining moisture in the skin.
- Poor skin barrier function due to other reasons.
- Overactive immune response to minor irritants.
- Environmental pollutants and allergens.
- Emotional stress.
Eczema Symptoms
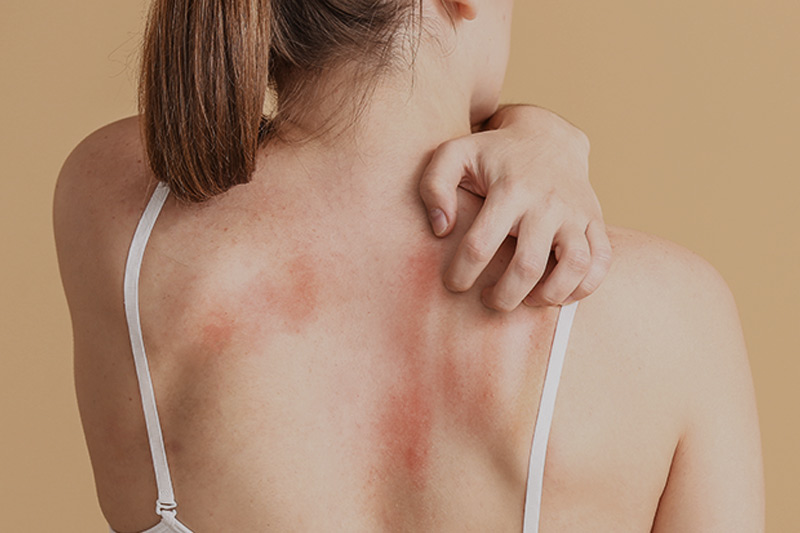
Eczema patients experience one or a combination of the following symptoms:
- Dry skin
- Intense itching
- Cracked skin (often due to scratching)
- Blisters
- Oozing fluid
- Crusts
- Redness
- Rashes
- Scaling
- Bumps
- Patches of rough, leathery skin
- Hyperpigmentation
- Fevers and chills
- Swelling
- Burning sensation
The manifestation of these symptoms often varies depending on the patient’s age. The following table summarizes the differences in typical symptoms among infants, children, and adults.
| Infants (0-2 years) | Children (2-12 years) | Adolescents and adults (over 12) | |
| Typical symptoms | Severe itching, rash, redness, oozing, crusting. | Itching, rash, red lesions, scaly, dry skin. | Itching, dry, thick skin, pain, skin discoloration. |
| Areas usually affected | Face, scalp, cheeks, sides of the arms and legs. In severe cases, the whole body. | Folds of the knees and elbows, neck, ears, wrists, ankles, around the eyes. | Face, hands, feet, neck. |
Who Can Get Eczema?
It is estimated that over 220 million people live with eczema. The highest rate of occurrence is in patients 1-5 years of age, but it can also develop in puberty and adulthood. It rarely occurs in people over 60. Statistics show eczema affects people of all races, nationalities, and sexes, but it is more prevalent in urban areas and developed countries.
Eczema Risk Factors
The following factors increase the risk of developing eczema:
- Family history of dermatitis and allergies.
- Living in cold areas with high humidity.
- Exposure to chemical irritants.
- Exposure to stress.
How Is Eczema Diagnosed?
There is no specialized test for eczema. The diagnosis is typically made by a dermatologist who examines the patient’s skin and medical history and asks questions about the severity and frequency of symptoms, when they occur, and related information. If the doctor can’t diagnose eczema with certainty, they may order additional tests, such as:
- Allergy tests to discover potential eczema triggers,
- Blood tests to discover conditions unrelated to eczema,
- A skin biopsy to confirm eczema.
How to Treat Eczema

Many children outgrow eczema as they get older. Other patients usually experience symptoms in unpredictable patterns. There isn’t a permanent cure, but available treatments can effectively reduce or eliminate symptoms and prevent flare-ups.
The treatments range from home solutions and natural remedies to prescription medication and cosmetic procedures.
How to Manage Eczema Symptoms
The effectiveness of a product or treatment depends on the eczema type, the severity of symptoms, and the patient’s behavior. Consistent skin care is essential in treating eczema.
Patients usually try several products and treatments until they find what works for them.
1. Prescription medications
Doctors prescribe antihistamines, anti-inflammatory drugs, topical steroid creams, and corticosteroids to reduce itching and swelling. They also prescribe immunosuppressants to help regulate the immune system.
Note: Find out what is the best anti-inflammatory skin care.
2. Moisturizers
Moisturizers are an essential part of eczema treatment. Patients need to moisturize regularly and whenever they feel their skin is dry. The best products for eczema include hypoallergenic hydrating creams labeled “for sensitive skin,” free of fragrances, dyes, and preservatives, and containing natural oils, lipids, and ceramides.
Note: Learn how to get rid of dry skin and which products to use.
3. Light therapy
Light therapy or phototherapy is a popular cosmetic treatment that uses UV light to reduce T-cells, which cause an inflammatory response. The treatment helps reduce redness, blemishes, pigmentation, and itching. It requires multiple sessions for effective results.
4. Holistic facials
A holistic facial is a gentler approach to alleviating eczema. It combines a massage with aromatherapy and plant-based skincare products to enhance the skin’s natural ability to retain moisture and fight external irritants.
5. Lotion after a short lukewarm shower
Hot water and/or sitting in water for long periods of time can make dry skin worse. Taking a quick lukewarm shower is best, and it’s important to apply a hydrating lotion or cream right after toweling off when the skin is still damp. This will help keep the moisture locked in. Avoid harsh antimicrobial soaps and opt for an oil-based natural cleanser free of SLS and fragrance.
6. Relieving stress
Emotional stress is known to trigger or exacerbate eczema symptoms. Patients are encouraged to try various stress-relieving techniques, including:
- Yoga
- Meditation
- Breathing techniques
- Massage
- CBD oil
Note: Read our blog post on the best holistic eczema treatments to find more solutions to your stress-related skin problems.
7. Psychological help
Eczema patients may develop more severe symptoms due to constant scratching, pain, and dissatisfaction with their appearance. Patients who experience sleep problems and psychological distress benefit from seeing a therapist or a psychiatrist.
8. Healthy diet
Diet modification is an important factor in managing eczema symptoms. Common allergens and processed foods often trigger eczema flare-ups, so patients need to learn which foods to avoid, and which can help them improve symptoms. For example, fruits and vegetables are rich in vitamins that help reduce swelling and relieve itching. Omega-3 fats help relieve dry skin, and foods with probiotics and prebiotics (e.g., kefir, yogurt, onions, garlic) improve gut microbiota, helping to reduce the inflammatory response.
9. Other self-care tips
With time, eczema patients learn to avoid potential triggers, refrain from scratching, and properly care for their skin. If you have eczema, it’s best to avoid the following:
- Irritating chemicals in soaps, detergents, and other cleaning products (wear gloves when washing dishes and cleaning)
- Heat, cold, and low humidity (a humidifier is a good solution for those sensitive to dry air)
- Wool and synthetic fabrics
- Nicotine and alcohol
- Common food allergens
Eczema Flare-Ups: Common Triggers
The periods when eczema symptoms intensify are called flare-ups. They are usually triggered by different internal or external factors, including the following:
- Environmental stressors, such as cold, heat, dry air, and smoke
- Household products like soaps, shampoos, and detergents
- Makeup, skincare products, and perfumes
- Emotional stressors
- Infections and common colds
- Food allergens (usually peanuts, eggs, and dairy)
- Pollen, pet dander, dust mites
When to See a Doctor
If you experience recurring dry and itchy skin, you can manage the symptoms using moisturizing creams, ointments, and over-the-counter products for eczema relief.
Visit a dermatologist if:
- Your symptoms don’t improve.
- You experience more severe symptoms (blisters, pus, severe itching, pain, fever).
- You need help choosing the right products and treatments.
Eczema FAQ
The following are the most common questions people ask about eczema.
How Common Is Eczema?
Eczema is a worldwide public health problem. An estimated 220 million people suffer from eczema - up to 20% of children and up to 10% of adults. The condition is ranked 15th for non-fatal diseases and 1st for skin diseases globally.
Is Eczema Contagious?
Eczema is not contagious. An eczema patient cannot pass the disease on to anyone else. However, people around the world mistakenly perceive it as contagious and often stigmatize the affected person.
Does Eczema Hurt?
Pain is a potential eczema symptom, typically resulting from intense scratching until the skin cracks, bleeds, and hurts. The pain may disrupt sleep and lead to emotional problems.
Is Eczema an Autoimmune Condition?
Eczema is not an autoimmune condition. It does not involve the immune system attacking the body’s healthy tissues. However, the two conditions are related because the immune system plays a role in developing eczema, and treatments often involve its suppression.
Conclusion
Eczema is a complex disease that significantly impacts our wellbeing and quality of life. Though there is no cure, there are effective solutions that can alleviate symptoms. Learn to recognize and avoid eczema triggers and try different treatments until you find those that help you.
If you need help creating an effective treatment plan for eczema, our medical team at Vibrant Skin Bar will be happy to assist.



